Introduction
Robot assisted surgery, having evolved from a niche research area in the late 1980’s, now represents one of the fastest growing divisions in the medical technology industry. As innovations in this area have allowed the application of surgical robots to expand to a wider range of surgical specialties and procedures, many healthcare facilities are routinely examining and validating clinical outcomes, case efficiencies, and financial impact when adopting new technologies. The goal of this white paper is to bring together insights from various centers of excellence to provide insights into these examinations to provide best practices and other key learnings.

According to Fortune Business Insights, the surgical robotics market is anticipated to have a compound annual growth rate (CAGR) over 20% for the next half decade. (July 2019)
Bounty of Research
There is an abundance of research and evidence communicating the benefits of robot assisted surgery (RAS) – including faster recovery time and shorter hospital length of stay, reduced blood loss, improved overall patient outcomes, lower utilization of pain medication, and minimal scarring due to smaller incisions. Within these published articles and surgeon-led symposiums is the mention of the implementation of integrated table motion (ITM). ITM is software that enables synchronized movement between the arms and instruments of the surgical robot, a surgical table, and –by extension – the patient.
ITM is currently available through the da Vinci Xi® System, which is wirelessly paired with a specific surgical table, the Hillrom TS7000dV Table. Today, over 85% of US da Vinci Xi Systems include Integrated Table Motion; therefore, to obtain a specific view of the impact of ITM on workflow and clinical outcomes, research was conducted to compare experiences using ITM vs. procedures that utilize a fixed surgical table from case start to case stop.
Study Demographics
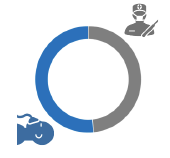
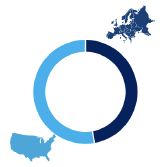
91 total respondents representing facilities in North America and Europe
Study Background
To answer this question of dynamic repositioning during a robotic-assisted surgical case versus an immobile, fixed position, SUAZIO Consulting conducted a two-phase study with over ninety hours of interview time with robotics surgeons and anesthesia team members (94% anesthesiologists and 6% CRNAs) to uncover insights from various centers of excellence, that represent academic, public, and private facilities from North America and Europe. Questions addressed topics related to providing care from either a fixed, immovable surgical table or one that can be repositioned intraoperatively with ITM. The feedback and data were analyzed over the course of the two qualitative studies conducted in the summer and winter of 2020.
Respondents first identified how frequently they utilize ITM and for which clinical specialties. Over two-thirds of the respondents utilize ITM in more than half of all cases, with the representation of clinical specialties as follows: urology (26%), general/bariatric (21%), colorectal (16%), gynecology (15%), and cancer (10%). ITM usage is consistent across specialties as are the contributing benefits to RAS procedures, with the key positive factors being workflow efficiencies and time-savings (37%), improved positioning and visualization (28%), improved communication and feedback (15%), safety (13%), and decreasing risk of contamination (3%). This paper will explore these top four categories: workflow, visualization, communication, and safety.
Workflow Efficiencies
When discussing workflow efficiency related to ITM, the most frequently cited aspect is the avoidance of undocking and redocking of the surgical robot. By eliminating this step, respondents provide a range of 10 to 35 minutes saved per procedure (range varies due to numerous types of procedures).
According to respondents, without ITM, the undocking process is needed for several reasons: when the table and patient require repositioning to target anatomy; for better visibility when organs obstruct the view; for longer cases when physiologic respiratory stress needs to be managed; or if the initial setup was not adequate. Less complex cases on average experience time savings of nearly 15 minutes. The complexity of the case and the experience of the surgical team can lead to high average time savings.
Study participants record average RAS case durations between two to four hours. Surgeons report nearly one of every four cases exceeds four hours, whereas anesthesiologists report this as nearly one in three. When asked what factors contribute to longer cases and how do the surgeons manage those cases with prolonged patient positions, catalysts for longer RAS include:
| – Amount or degree of cancer – Frequent instrument change – Tumor attachment to other structures – Advanced disease – Size and location of tumor – High patient risks, patient health – Adhesions, scare tissue |
– Imaging quality capturing internal structure – Bleeding – Prior surgeries – Patient obesity – Dissection – Complexity of procedure – Anastomosis challenges – Issues removing specimens |
Anticipated or not, longer case durations with a fixed, single position (without ITM) may require additional and modified behaviors involving either undocking to level the patient and adjusting their hemodynamic responses and ventilation parameters, heightening the level of communication amongst the team, conducting pre- and post-planning sessions, and/or by restricting fluids. By contrast, with ITM, the wirelessly paired surgical table is leveled out with the robotic arms still docked and the surgeon continuing to operate while the patient’s parameters normalize, saving valuable time and avoiding the distraction from the interruption of undocking.
Maintained focus and concentration were subtle advantages mentioned by 76% when forgoing the undocking process. Some of the surgeons even report not having to be as selective with their case choice or optimal patient candidates, knowing ITM can overcome positioning barriers and complications.
In Their Own Words
“It’s a matter of gravity for all of the cases and why I need to do it. Certain parts of the dissection, I need access to the specific parts of the body. ITM allows me to move intestines that creep into the dissection I’m working on without needing an assisting hand.”
– Surgeon, USA
“If we are having a really hard time ventilating the patient, with the older system, we have to completely dislodge the robot, move and see what happens. With the new system, you can take them out of Trendelenburg.”
– Anesthesiologist, USA
“The ability for the entire team to focus on the procedure and do away with all the cumbersome and inefficient actions that require and undocking and redocking.”
– Surgeon, UK
“(We) were willing to settle for a close to good enough positioning because we didn’t want to waste the time to position the patient again.”
– Anesthesiologist, USA
Enhanced Visibility and Access
Surgeons rank enhanced visibility and access granted as the second most critical benefit from ITM. They describe how the adjustment of angles, applying more Trendelenburg, reverse Trendelenburg, and/or tilt during the case provides critical views and access to the surgical site as gravity from the table movement moves organs out of the way.
Enhanced visibility is expressed for large, multi-quadrant procedures – for example, mobilizing the colon for a tension-free anastomosis or navigating narrow, tight spaces in gynecology and urology cases to pull anatomy down and out of the way to make small discrete movements. In addition to target anatomy exposure, intraoperative re-positioning is attributed to locating unanticipated bleeding and critical, anatomical structures to avoid.
Surgeons share how even slight movements assist with optimal line of sight and suturing with a clearer view. Many surgeons speak of how they do not have to “settle” or “compromise” on a preferred approach, angles, or views as they would with a non-movable table.
In Their Own Words
“One thing that has helped us is being consistent with having the appropriate level of tilt, particularly for hysterectomies and prostates.”
– Anesthesiologist, USA
“Prior to the new robots with the integrated table motion, without the numbers in front of me and anecdotally, the conversion rate from RAS to open surgery was absolutely higher.”
– Anesthesiologist, USA
“(ITM) creates less confusion, fewer mistakes, and less room for error.”
– Surgeon, USA
Feedback Enhanced Communication & Focus
A third, top-favored outcome from Integrated Table Motion is the enhanced communication – although the attributing source of the outcome varies. Both surgeons and anesthesia team members equally value data feedback received from the paired communication with the surgical robot and surgical table. From the surgeons’ points of view, the surgical table’s positioning status and degrees of angles displayed in their console help them to standardize success and reproduce positive outcomes.
Surgeon respondents describe the power in positioning with specific numerical values and not subjective terms such as “a little more.” The anesthesia team respondents also appreciate the more “precise” and “smooth” communication between themselves and the surgeons. Aside from the quantifiable information provided by the surgical table to the surgical team, another form of improved communication is the removal of emotional barriers. Having ITM eliminates worry and stress in knowing the initial setup could be adjusted, a better angle could be achieved intraoperatively, and if complications arise, the patient can be repositioned without halting the surgical case, losing focus or workflow efficiency.
In Their Own Words
“Prior to ITM, it was a conversation and more subjective instead of looking at numbers.”
– Anesthesiologist, USA
“Everything is synchronized. It is more convenient, and it is much more pleasurable to work in the ITM environment.”
– Anesthesiologist, UK
“Communication works well. There is a good flow of information. All of these things helps lead to better clinical outcomes, excellent vision, and faster recuperation.”
– Surgeon, Switzerland
“[Without ITM] I’m always afraid of too much manipulation of the bowel, with robotic arms especially for fear of enterotomy.”
– Surgeon, USA
Outcomes of Safety and Sterility
The study produced unforeseen outcomes from the surgeons’ feedback when comparing the ideal state using Integrated Table Motion versus the older ways without ITM or when not having access to the TS7000dV, the surgical table model exclusively compatible with da Vinci Xi System with ITM.
Advantages include low to zero conversion rate to open surgery, elimination of an extra port in many cases to assist with manipulations or an extracorporeal anastomosis since additional gravity shifts provide the manipulation and intracorporeal anastomosis is more feasible, less manipulation of the intestines, and less trauma to the organs, minimizing the fear or possibility of an unintended enterotomy or iatrogenic injury since gravity moves the internal organs. Lower on the list of prioritized benefits, as stated by one of several surgeons, is “the decreased utilization of extra instruments — which in the robotic world, the more instruments, the more cost it puts in the procedure. Not having to use things to retract because you’re able to move the bed and allow the anatomy to move.” Finally, just as the communication with ITM is described as seamless and without tension, this translated to several surgeons and anesthesiologists in a more physical way.
Many described their operating rooms having enhanced sterility due to the lack of commotion and movement. As one respondent states, “Your overall sterility is improved when you have people and instruments staying in the sterile field for the entirety of the case and not moving about disconnecting instruments, undocking and moving equipment around.” Additional commentary suggests less conversion to open or laparoscopic procedures also helps maintain a more sterile environment. This is an interesting point to consider in a future study.
Conclusion
Robotic-assisted surgery with Integrated Table Motion has provided surgical teams with new confidence in addressing longer and more complex procedures. The adoption of Integrated Table Motion with the Hillrom TS7000dV surgical table (formerly known as the Trumpf Medical TruSystem 7000dV Table) has further enhanced operations to achieve clinical, operational, and financial benefits and expand the scope of what a facility can address in a safer, more efficient way. Being able to reposition the surgical table intraoperatively has many positive contributions and is a convincing choice to use an assist from gravity in robotic-assisted surgery.
References
1) Hongyi Liu, Maolin Xu, Rong Liu, Baoqing Jia, Zhiming Zhao. The Art of Robotic Colonic Resection: A Review of Progress in the Past Five Years, 2020.
2) Fortune Business Insights. Surgical Robots Market Size, Share, and Industry Analysis by Application, By End User, & Regional Forecast 2019-2026, 2019
Acknowledgements
The participants for this research were invited based on their level of experience with robot assisted surgeries. These participants volunteered their time for this effort, and their expertise accounts for a major source of the material.
SUAZIO is an expert in medical devices and diagnostics strategic insights creation.
If you are interested to learn more about this data, please contact Fred Shelly, Project Director at SUAZIO, f.shelley@suazio.com, +1-215-987-5884 or Christophe Van der Linden, CEO, c.vanderlinden@suazio.com



